Platelets are blood cells that cause blood to clot and contain growth factors. Doctors use these proteins to promote healing in musculoskeletal injuries and conditions. For more information, click the Prp San Diego to proceed.
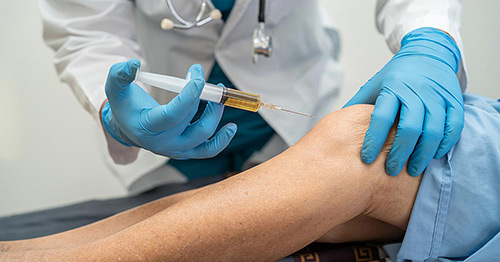
PRP injections are made by drawing a small amount of blood from a vein in your arm. Then, the doctor runs it through a centrifuge, which separates blood components based on density.
Platelets are one of the most versatile and complex cell types in the body. Their primary function is to initiate blood clot formation, and platelet-rich plasma contains high concentrations of these cells. When PRP is injected, it alters the microenvironment of the injury site by upregulating anabolic pathways, modulating the inflammatory response and promoting stem cell differentiation into tissue-specific cells. This combination of pro-inflammatory and anti-inflammatory mediators and cell differentiation promotes bone regeneration, muscle healing and tendon injuries, and enhances vascularity.
During injury, platelets respond quickly by adhering to exposed endothelium and activating with physiologic agonists (like collagen, vWF and ADP) causing a shape change that allows for rapid release of cytoplasmic substances like coagulation factors and platelet-derived growth factor (PDGF). The PDGF promotes the proliferation of fibroblasts, smooth muscle cells, osteoblasts and keratinocytes and aids in wound healing, extracellular matrix production and angiogenesis. VEGF, a potent angiogenic growth factor also found in platelets, stimulates angiogenesis in the wounded area and may contribute to the regeneration of meniscal tears, ligament and tendon injuries and other conditions with poor vascularity.
Once a platelet is activated, it releases a number of inflammatory mediators including arachidonic acid, leukotrienes, prostaglandins, and lipoxins. These mediators can promote or inhibit inflammation and have been shown to decrease pain and swelling in patients with arthritic knees after LR-PRP treatment.
In addition to inflammatory mediators, platelets also secrete a variety of immunomodulatory agents that affect the innate and adaptive immune system. The chemokine receptors p-selectin, CD40L and RANTES allow platelets to interact with leukocytes, regulating their chemotaxis and activation. Platelets can also release soluble mediators that enhance the phagocytic activity of monocytes, as well as modify their effector functions by activating NF-kB and increasing the expression of cytolytic enzymes.
Platelets are also able to modulate the proliferation and differentiation of fibroblasts, smooth muscle cells and osteoblasts through transforming growth factor-beta (TGF beta) and insulin-like growth factor-1 (IGF-1). In addition, platelet adenosine triphosphate activates dendritic cells by binding to P2Y12, which increases antigen uptake and leads to DC maturation and increased antibody generation.
Platelet-rich plasma contains many more platelets than are typically found in blood. This allows for a higher concentration of growth factors, which play a key role in tissue repair and regeneration. PRP is used to treat conditions such as strained tendons, meniscus tears and osteoarthritis. It can also be injected into the skin for hair rejuvenation and other cosmetic uses.
Platelets are nucleated discoid cellular elements that develop from bone marrow and circulate in the blood. They are best known for their role in clotting blood, but they also secrete several important growth factors and other bioactive compounds that can promote cell regeneration and tissue healing.
The tissue healing process involves a complex clotting cascade, in which platelets are activated upon interaction with the extracellular matrix of damaged tissues and release a number of important proteins. These proteins are released from a variety of secretory granules present in platelets, including dense and alpha granules, leukocytes, and fibrinogen. These molecules induce a platelet plug formation, clot lysis, and the forming of a fibrin meshwork that promotes healing.
These biological activities are induced by the cytokines and other growth factors contained in the platelet-rich plasma. Moreover, platelets also contain other enzymes that help in the degradation of dead cells and in the clotting process.
Another component of the PRP is leukocytes, which are immune system cells that can enhance the tissue healing process by releasing pro-inflammatory cytokines and suppressing the growth of some bacteria.
The process of creating PRP involves obtaining blood from the patient and then spinning it in a centrifuge to separate the red blood cells from the platelets and other leukocytes. Once the PRP has been separated, it can be injected into the treatment site.
Platelet-rich plasma, or PRP, is blood that contains concentrated amounts of platelets. Platelets are blood cells that help to form clots and play an important role in wound healing. When injected into a patient’s body, the concentrated platelets release growth factors and other substances that stimulate and accelerate the healing process of injured tissues.
Medical professionals collect a sample of a patient’s blood and place it in a device called a centrifuge, which spins at such high speeds that the plasma separates from the red and white blood cells. This concentrates the platelets within the plasma, which can then be extracted and prepared for administration.
Several different kits for preparing PRP are available. These differ in the speed, temperature, and anticoagulant used for centrifugation. These factors can affect the platelet concentration and thus impact the results of clinical studies evaluating the efficacy of PRP therapy.
The platelets in PRP contain a wide variety of bioactive molecules, including adhesive proteins, cytoplasmic granules, growth factors, chemokines, vascular endothelial growth factors and more. These are released from the granules in response to injury, increasing cell growth, proliferation, fibrosis, and angiogenesis.
PRP can be used alone or in combination with other musculoskeletal treatments, such as laser, microneedling and PDO threads. Your doctor may recommend it for treating chronic pain, sports injuries, tendonitis and other musculoskeletal issues.
After a treatment session, you can expect some soreness at the injection site for a few days. Your doctor will likely recommend that you avoid anti-inflammatory medications after a PRP injection, as it can block the body’s natural inflammatory response to heal the site.
PRP is a relatively safe treatment when performed by a certified physician. However, as with any procedure, it has risks and complications. Your doctor will discuss the potential side effects and benefits of PRP therapy with you before recommending it for your specific condition or injury.
Platelet-rich plasma is a treatment that uses your own blood to accelerate healing in a specific area. It contains a high concentration of platelets, which are best known for their role in blood clotting, but also contain proteins that trigger cell reproduction and stimulate tissue regeneration.
To produce PRP, clinicians use a small sample of your own blood and place it in a centrifuge. This spins the sample, separating out the other components of your blood and creating a solution with a higher concentration of platelets than normal.
Platelets can be used to treat a number of different conditions, including chronic tendon disorders. They can be injected into a joint to reduce pain and swelling from arthritis or to heal a tendon injury. The platelets release growth factors that promote healing, and they also contain a substance called hyaluronic acid, which increases collagen production and helps restore flexibility to joints.
Clinical trials have shown that PRP injections are a more effective treatment for chronic tendon disorders than other types of injections, such as corticosteroid shots. Unlike steroid injections, which suppress the immune system at the injection site, PRP is non-invasive and does not weaken collagen structures at the injury site.
In addition to the treatment of painful joints and tendons, PRP can be used to improve skin health. The high concentration of growth factors in the PRP can help to improve skin elasticity and slow down signs of aging, such as fine lines and wrinkles.
Because the PRP comes from your own body, there is no risk of rejection or allergic reaction. It is also a much safer alternative to dermal fillers, which are made from foreign materials.
Currently, PRP is being used to treat a variety of injuries and conditions, from sports injuries to hair loss. It is an exciting new field in regenerative medicine, and we are excited to be a part of it! If you are interested in learning more about how our team at Memorial Healthcare System can help you, contact us today! We offer a wide range of orthopedic and regenerative services, including PRP therapy.